Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
Maybe it’s my age or my tenure in the LTC field the past 40+ years. I found this Thirty-Year Trends in Nursing Home Composition and Quality Since the Passage of the Omnibus Reconciliation Act study published in JAMDA (Journal of the American Medical Directors Association) to be a fascinating read. Like a trip down memory lane in 7 pages. The following quotes set the stage:
“The purpose of this study was to summarize changes in the NH industry in the 30 years since the seminal regulatory change affecting NHs. Specifically, we use historical data from 3 national sources and describe changes in NH facility characteristics, resident characteristics, and quality of care from 1985 through 2015. The 30th Anniversary of OBRA provides a unique opportunity to examine the changes within this vitally important industry. This article can aid in understanding long-term trends, as well as provide insight into what changes we might expect in the future.”
“OBRA 1987 created regulations for NHs in an effort to improve the quality of care delivered to residents. OBRA included a minimum set of care standards and rights for people residing in Medicare- and Medicaid-certified NHs. OBRA 1987 had a focus on residents’ quality of life and care, expectations for improved or maintained resident health, as well as residents’ rights to banking, organized family councils, and freedom from unnecessary physical and chemical restraints. The Act also standardized certification standards and enforcement strategies. As such, OBRA 1987 was an overhaul of the NH industry and marked a new beginning for NH care and regulation.”
I worked in the trenches, literally and figuratively speaking, of LTC pre and post-OBRA ’87. I remember pre-OBRA very well and I lived through and thrived/grew in my nursing profession courtesy of OBRA ’87. Those were interesting times, as one could say about the RoPs, etc. that we are experiencing now.
What does this study show? (Note that the study concluded in 2015 – before the RoPs were fully implemented. RoPs are the 1st rewriting of LTC standards since OBRA ’87.)
- In the past 30 years, the NH industry has decreased in size, from 19,068 facilities in 1985 to 15,686 in 2016.
- There has also been an increase in the percentage of facilities that are nonprofit (25% in 1985 and 31% in 2015) and that are dually certified by both Medicare and Medicaid (33% in 1985 and up to 97% 2015).
- Between 1995 and 2015, chain membership increased from 51% to 57%.
- The percentage of facilities with an Alzheimer’s special care unit increased from 11% to 15% and
- Overall NH occupancy rates declined from 87% to 81%.
Regarding make-up of residents:
- Average age of residents has remained constant.
- The percentage of residents who are racial and ethnic minorities has increased from 7.8% in 1985 to 20.7% in 2015.
- Average percentage of females decreased from 72% of residents in 1985 to 67% in 2015.
- The prevalence of long-stay residents within NHs has remained stable at 69% of all residents over this time period.
- Percentage of residents admitted from the hospital increased from 67% in 2000 to 85% in 2015.
- Between 1992 and 2015, the average percentage of residents with Medicaid as a primary payer decreased from 64% to 58%, whereas the average percentage of residents with Medicare as the primary payer rose from 9% to 15%.
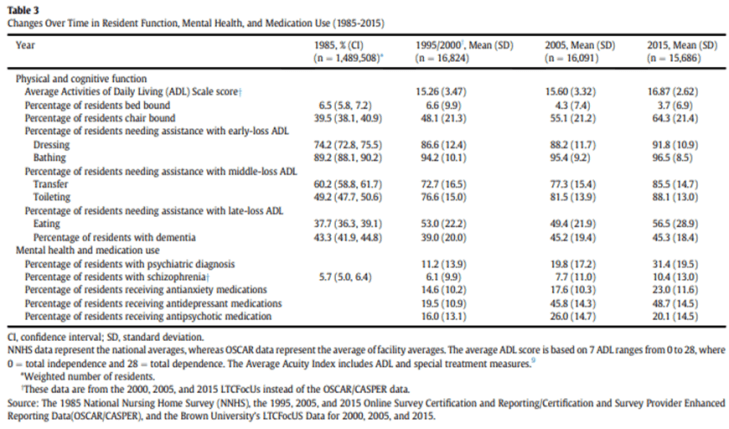
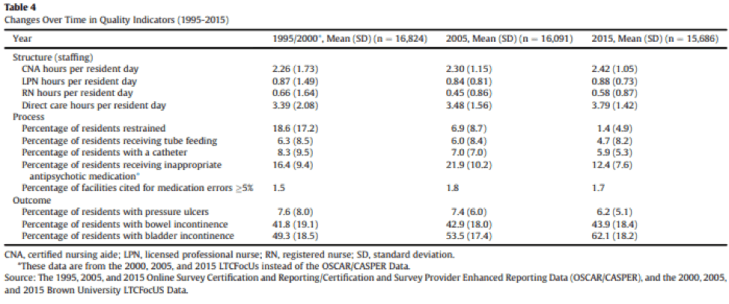
This study is rich in the data it provides. Consider the study’s statement of Conclusions and Implications:
“Overall, OBRA 1987 is positively associated with the quality of care improvements in NHs despite increasing impairment of NH residents. OBRA 1987 was also successful in implementing and enforcing the MDS resident assessment survey, and without that this research would not be possible. Because of the aging-in-place movement, we are seeing lower occupancy rates in NHs. Older adults without financial resources, disproportionality minority older adults, are becoming an increasing proportion of NH residents, as they may not be able to as readily access these care alternatives. Current and future policies should focus on expanding equitable access to the remaining long-term care services and supports in the continuum of care, particularly given the policies and initiatives focused on decreasing NH utilization through support of home and community-based alternatives. Although NHs continue to focus more on short-stay post-acute care residents and long-stay residents with dementia, more work will need to be done in community-based settings to ensure the highest quality care and life. Improving quality is also about improving equity, and it is important for future work to examine access to quality care for our most vulnerable older adults who are sometimes triply and doubly vulnerable because of their cognitive status, race, and/or socioeconomic position. As our work shows, much of the quality progress made in NHs has been because of regulation and oversight over the years. The same level of oversight does not exist for all community alternatives, but the evidence presented here is indicative of effective practices.
Future research is also needed to understand whether these improvements in quality over the past 30 years have been equitable on the basis of race, socioeconomic status, gender, and geography. In sum, our findings document the 30-year history of NHs since the passage of the seminal legislation: OBRA 1987. As we look toward the future of long-term care, it is important that we reflect on the past.”
I encourage you to read and share this study. It certainly is food for thought – past, present and future. What will LTC look like in another 10, 15 or 30 years? What can we do today, individually as well as collectively, to ensure the highest quality of care and life for our most vulnerable citizens?
