Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
On March 17, 2020, CMS announced that it has “broadened access to Medicare telehealth services so that beneficiaries can receive a wider range of services from their doctors without having to travel to a healthcare facility. These policy changes build on the regulatory flexibilities granted under the President’s emergency declaration. CMS is expanding this benefit on a temporary and emergency basis under the 1135 waiver authority and Coronavirus Preparedness and Response Supplemental Appropriations Act. The benefits are part of the broader effort by CMS and the White House Task Force to ensure that all Americans – particularly those at high-risk of complications from the virus that causes the disease COVID-19 – are aware of easy-to-use, accessible benefits that can help keep them healthy while helping to contain the community spread of this virus.”
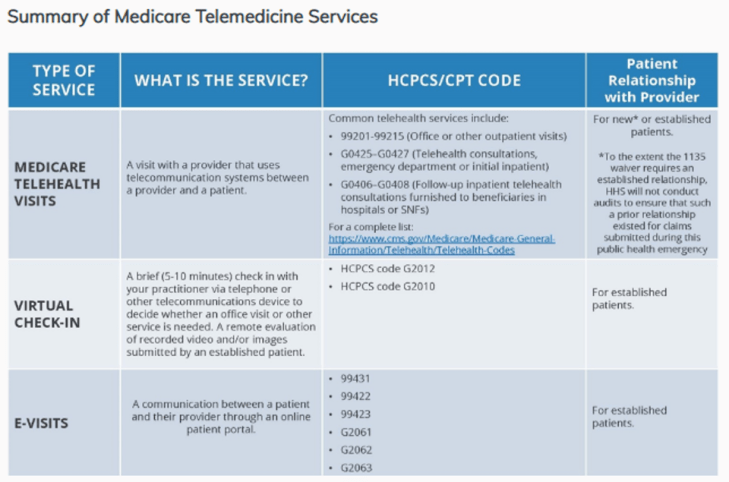
You can read this and more in the Medicare Telemedicine Health Care Provider Fact Sheet. The Fact Sheet includes information about the 3 types of virtual services:
- Medicare telehealth visits
- Virtual check-ins
- E-visits
There is a lot of information in this Fact Sheet. Please review and share with your team as well as physicians that care for residents in your facility/community.
Medicare Telehealth Frequently Asked Questions (FAQs) is a 4-page document that you’ll also want/need to review.
Additionally, you should be aware of this directive as well:
HEALTH INSURANCE PORTABILITY AND ACCOUNTABILITY ACT (HIPAA): Effective immediately, the HHS Office for Civil Rights (OCR) will exercise enforcement discretion and waive penalties for HIPAA violations against health care providers that serve patients in good faith through everyday communications technologies, such as FaceTime or Skype, during the COVID-19 nationwide public health emergency. For more information: https://www.hhs.gov/hipaa/for-professionals/special-topics/emergency-preparedness/index.html.
