Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
AS RESIDENT POPULATION SHRINKS, NURSING HOMES REMAIN UNDERSTAFFED is the “subtitle” of the alert email I received on Friday, January 22, 2021 from the Long Term Care Community Coalition.
January 22, 2021 – Staffing levels are a key predictor of nursing home resident outcomes during the COVID-19 pandemic. Studies show that facilities with staffing shortages have been more susceptible to COVID-19 outbreaks, resident deaths, and other negative resident outcomes. A sufficiently staffed nursing home is not only better prepared to prevent the spread of infections but can also protect its residents from the devastating effects of isolation and neglect.
Today, LTCCC announces the publication of the latest user-friendly data on staffing for every U.S. nursing home (in compliance with mandatory reporting requirements). The latest federal data indicate that U.S. facilities remained understaffed during the 3rd quarter of 2020, averaging 3.43 total care staff hours per resident day (HPRD) and 0.47 RN care staff HPRD. The nationwide averages fall short of the amount of time needed to ensure that residents receive clinical care (4.10 total care staff HPRD and 0.75 RN HPRD), according to a landmark 2001 federal study. Meanwhile, nursing homes have experienced a drastic decline (12.2%) in resident population nationwide since the start the of the pandemic. Despite receiving billions of dollars in COVID relief aid, too many facilities are failing to invest in the staffing required to meet their residents’ needs.
LTCCC’s Q3 2020 staffing report provides easy-to-use files for every state that include: 1) The levels of care staff; 2) Staffing levels for important non-nursing staff, including administrators and activities staff; and 3) The extent to which the facility relies on contract workers to provide resident care.
Staffing Facts for Q3 2020:
- Total care staff and RN HPRD (3.43 & 0.47) plateaued from the previous quarter (3.46 & 0.45).
- The average facility census has declined 12.2% since the start of the pandemic—from 86.6 in Q4 2019 to 76.0 in Q3 2020. The census decline is accompanied by a slight increase in total care staff HPRD (1.6%) and a more significant increase in RN HPRD (9.9%) since Q4 2019.
- Top five states for total staffing HPRD: Alaska, Oregon, Hawaii, California, Vermont.
- Bottom five states for total staffing HPRD: Missouri, Texas, Oklahoma, Illinois, South Dakota.
Note: LTCCC’s Q3 2020 staffing report differs from previous reports by including additional staffing categories: RN Administrative (RN Admin), RN Director of Nursing (RN DON), Physician Assistant, Nurse Practitioner, Speech/Language Pathologist, Occupational Therapy, and Physical Therapy.
A full version of this alert can be found on our website at https://nursinghome411.org/alert-staffing-q3-2020/.
This is what the report website looks like when you initially enter:
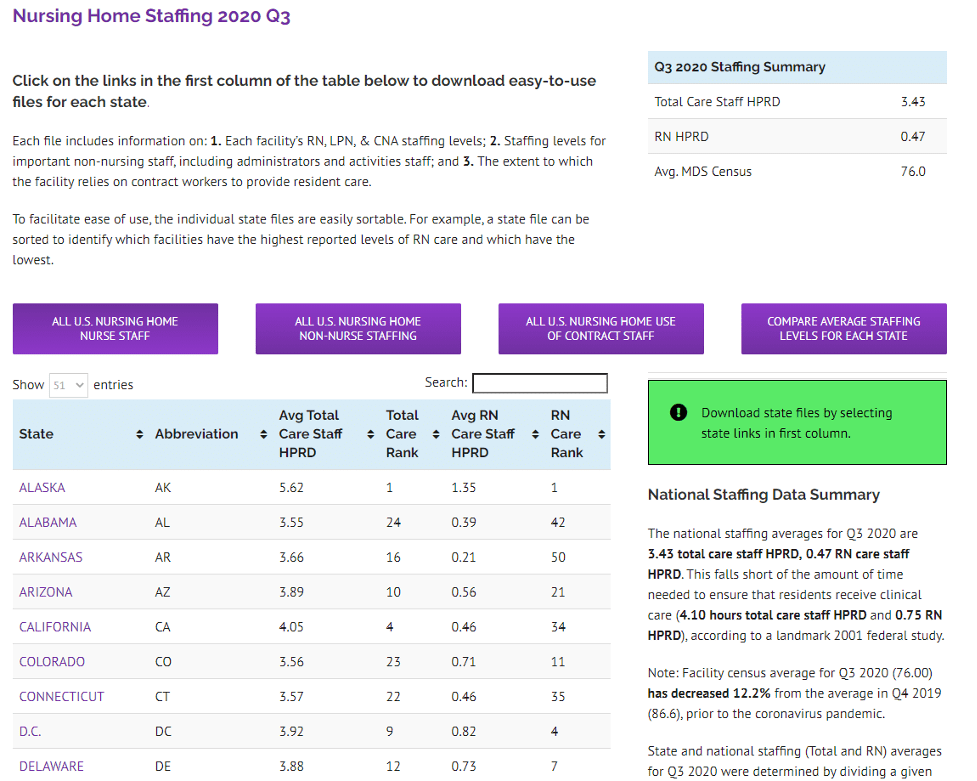
There’s a huge amount of data to be viewed and analyzed. I encourage you to take a look at the information, starting with your state and your facility(ies).
Notes on the Information Provided
- Data provided are the averages for the quarter (three-month period).
- If a facility is not listed, it has not provided appropriate staffing data to CMS.
- The state and national staffing averages provided on our website do not include staff time designated for administrative or non-care functions. They only include the staff that nursing homes have designated as providing resident care. Though this report includes RN Admin and RN DON data, those data are excluded from state and national staffing averages.
- See the Notes and Glossary tabs in each file for more information about the data.
To access staffing reports from previous quarters, visit LTCCC’s Staffing Page.
If you’re not familiar with the LTCCC, here’s their mission statement (hyperlink to that webpage is found in the 1st paragraph of this blog; there’s additional information on that website as well):
“The Long Term Care Community Coalition (LTCCC) is a nonprofit organization dedicated to improving quality of care, quality of life and dignity for elderly and disabled people in nursing homes, assisted living and other residential settings.
LTCCC focuses on systemic advocacy, researching national and state policies, laws and regulations in order to identify relevant issues and develop meaningful recommendations to improve quality, efficiency and accountability. In addition to providing a foundation for advocacy, LTCCC uses this research and the resulting recommendations to educate policymakers, consumers and the general public. Consumer, family and LTC Ombudsman empowerment are fundamental to our mission.
LTCCC’s work is grounded in its organization as a New York State based coalition of consumer, community, civic and professional organizations, bringing together these different stakeholders to identify & address the systemic issues that affect quality of care and dignity in long-term care.
LTCCC is proud to host two local LTC Ombudsman Programs in New York: the Hudson Valley LTC Ombudsman Program and the Tri-County LTC Ombudsman Program.”
