Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
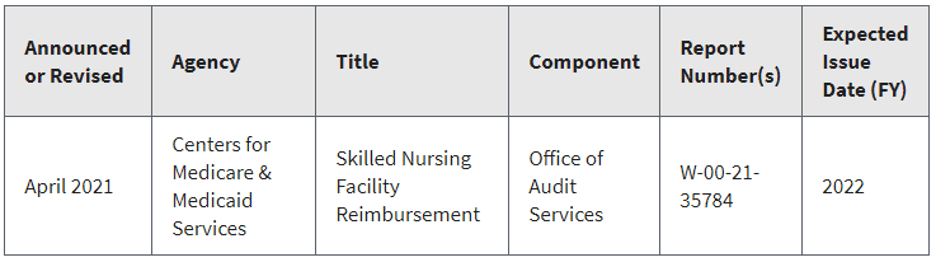
OIG (Office of Inspector General) has added SNF reimbursement to its work plan this month.
A skilled nursing facility (SNF) is a nursing home that provides skilled nursing care and rehabilitation services such as physical, speech, and occupational therapy to beneficiaries who need assistance after hospitalization. In October 2019, the Centers for Medicare & Medicaid Services (CMS) implemented a new payment system for determining Medicare Part A payments to SNFs. Specifically, CMS implemented the Patient Driven Payment Model (PDPM), a new case-mix classification system for classifying SNF patients in a Medicare Part A covered stay into payments groups under the SNF Prospective Payment System. Under PDPM, payment is determined by factoring in a combination of six payment components. Five of the components are case-mix adjusted and include a physical therapy component, an occupational therapy component, a speech-language pathology component, a nontherapy ancillary services component, and a nursing component. Additionally, there is a non-case-mix adjusted component to cover utilization of SNF resources that do not vary according to patient characteristics. We will determine whether Medicare payments to SNFs under PDPM complied with Medicare requirements. (This statement is found here. Bolding added by me.)
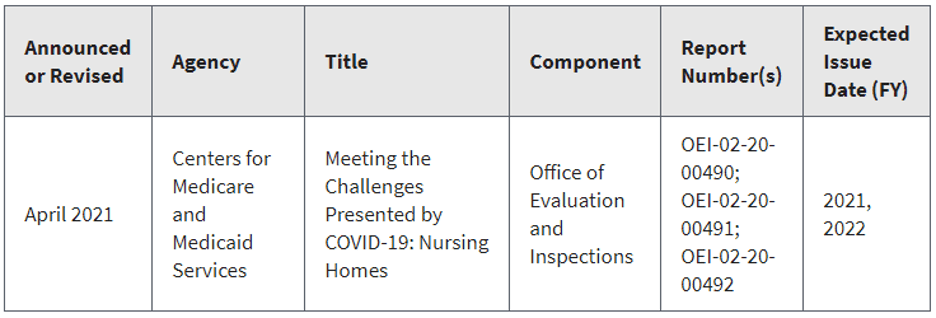
On the subject of OIG and its active work plan, this report is due for publication in either FY2021 or FY2022 – Meeting the Challenges Presented by COVID-19: Nursing Homes.
Nursing homes have been at the epicenter of the COVID-19 pandemic. Residents in these homes have been particularly affected by the disease, as they are predominantly elderly individuals who have underlying medical conditions and live in close quarters. To prevent and mitigate future outbreaks, it is important that we understand how nursing homes experienced the COVID-19 pandemic. This nationwide, three-part study will examine how the pandemic affected nursing homes. The first part will analyze the extent to which Medicare beneficiaries residing in nursing homes were diagnosed with COVID-19 and describe the characteristics of those who were at greater risk. The second part will describe the characteristics of the nursing homes that were hardest hit by the pandemic (i.e., homes with high numbers of beneficiaries who had COVID-19). The third part will describe the strategies nursing homes used to mitigate the unprecedented challenges of COVID-19. These challenges include procuring critical supplies, testing residents and staff, isolating high numbers of contagious residents, caring for those afflicted, and protecting residents and staff on a scale never before experienced in this country.
I’ll be watching for these 4 reports and will post when available.
