Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
“GAO was asked to examine SNF staffing and rates of critical incidents. This report
[published August 9, 2021 … 63 pages; Highlights found here]
examines (among other objectives): SNF performance on staffing measures, CMS reporting of staffing information on Care Compare, and Medicare payments for critical incidents. GAO analyzed CMS staffing and critical incidents data, information on Care Compare, and Medicare claims data for 2018 and 2019. GAO also interviewed CMS officials and other stakeholders such as key researchers and beneficiary groups.”
What GAO (Government Accountability Office) found:
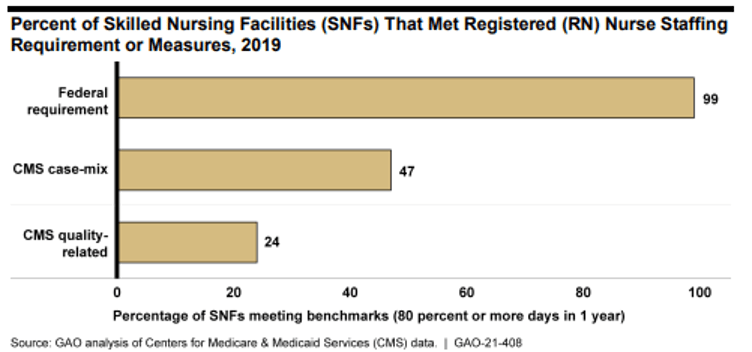
- Analysis of 2019 staffing data found that almost all SNFs frequently met a federal requirement for a registered nurse (RN) on site for 8 hours per day
- About half of SNFs frequently met Centers for Medicare & Medicaid Services (CMS) case-mix measures—hours worked per resident that vary based on the medical needs of each SNF’s residents—that CMS uses to set SNF staffing ratings
- About one-quarter of SNFs frequently met staffing thresholds for minimum RN and total nurse staffing that a CMS staffing study identified as needed to avoid quality problems. SNFs are not subject to these quality thresholds for ratings or as requirements, but many stakeholders have recommended that they be used as SNF staffing thresholds.
“CMS reports certain key staffing information—such as RN overall staffing hours—on its Care Compare website, but does not report other important information. For example, GAO found that average RN staffing hours decreased about 40 percent on weekends, but CMS does not directly report this information. This limits the ability of beneficiaries to make informed choices among SNFs when choosing a facility. GAO estimated that in 2018 Medicare spent over $5 billion on critical incidents that CMS defines as potentially preventable—which are mostly about 377,000 hospital readmissions occurring within 30 days of the SNF admission. Current law directs CMS to make reductions of up to 2 percent to certain SNFs’ payments to incentivize them to improve care, but does not address additional reductions. Experts have noted that payment incentives under current law may not be sufficient to motivate SNFs to improve their staffing, which in turn could lead to reductions in critical incidents. Without stronger payment incentives, Medicare is unlikely to reduce the billions in spending on potentially preventable critical incidents or the patient harm that can occur from them.”
I encourage you to review this report with your team. Take a look at the data in the Appendices. Where does your facility fit in the GAO analysis? PBJ data was used for this analysis.