Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
It’s that time of year (no, not Christmas/the holidays just yet) – flu season.
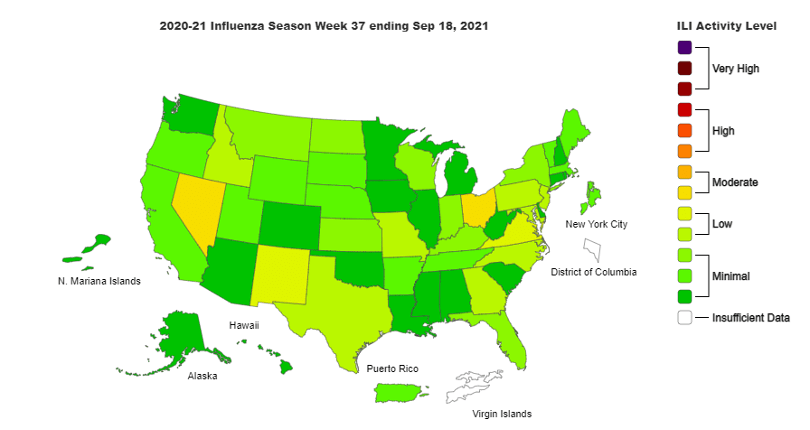
[1] As you can see from the above CDC map, the states of Nevada and Ohio are already reporting moderate flu activity. We can expect this map to get more colorful as the weeks pass – much like the fall colors. Unlike those fall colors we love, flu activity can be deadly. “The annual burden of influenza in the United States is significant, leading to 140,000-810,000 hospitalizations and 12,000-61,000 deaths each year since 2010.”[2] That was true until last year. From September 28, 2020, to May 22, 2021, only 0.2% of respiratory specimens tested were positive for the flu, compared to the three seasons prior when test positivity peaked between 26.2% and 30.3%. The cumulative rate of flu hospitalizations in 2020-21 was the lowest recorded since data collection began in 2005. The U.S. saw about 700 deaths from influenza during the 2020–2021 season.[3][1]
What made last year unusually low for flu activity? COVID-19 mitigation measures such as wearing face masks, staying home, hand washing, school closures, reduced travel, increased ventilation of indoor spaces, and physical distancing, likely contributed to the decline in 2020-2021 flu incidence, hospitalizations and deaths. Influenza vaccination may also have (contributed) to reduced flu illness during the 2020–2021 season. Flu vaccine effectiveness estimates for 2020-2021 are not available, but a record number of influenza vaccine doses (193.8 million doses) were distributed in the U.S. during 2020-2021.
What’s the concern for this flu season? Since this past summer, many states have relaxed COVID-19 mitigation measures. States, as well as within individual states, have varying requirements/guidelines for public places such as schools, restaurants, entertainment venues. Masking, COVID-19 vaccination and distancing have become political footballs. Failure to follow these measures as well as hesitancy to be vaccinated continue to cost lives, now including the lives of our children. Variants continue to surface as the coronavirus continues to find willing and more than suitable hosts in unvaccinated individuals. If we continue to fail to follow proven medical and scientific advice, the death toll in the U.S. will sharply climb from both COVID-19 as well as influenza (flu). We will indeed have a “twindemic” instead of just the pandemic. Make no mistake, both are public health emergencies and they’re deadly.
The CDC recommends flu vaccine for everyone older than 6 months, unless an individual’s doctor has specifically recommended against the vaccine for him/her. Flu vaccines should be administered after August and before the end of October. People who are or might be pregnant should receive the flu vaccine as well. Get your flu shot NOW! Encourage your family, friends, coworkers, etc. to get the flu shot. The vaccine protects from serious infection that requires hospitalization as well as death. Skipping the flu shot, especially during the COVID-19 pandemic, is extremely risky and dare I say life-threatening. The CDC wants all Americans to understand that as the pandemic continues, increasing flu shot coverage is important to reduce the burden on the healthcare system, avoid exacerbation of existing health inequities and to maintain the public’s health.
If you haven’t gotten the COVID-19 vaccination yet, please consider doing so as soon as possible to avoid serious illness, hospitalization and/or death. The life you save may be your own and/or someone you love.
Have questions about either vaccine? Check out these references/resources:
- Frequently Asked Influenza (Flu) Questions: 2021-2022 Season
- Flu Information for Health Professionals
- Post-acute and Long-term Care Facility Toolkit: Influenza Vaccination among Healthcare Personnel
- About Flu
- Different COVID-19 Vaccines
- Myths and Facts about COVID-19 Vaccines
- Frequently Asked Questions about COVID-19 Vaccination
- Ensuring COVID-19 Vaccine Safety in the US
- Similarities and Differences between Flu and COVID-19

[1] https://www.cdc.gov/flu/weekly/index.htm
[2] https://www.cdc.gov/flu/fluvaxview/nifs-estimates-sept2020.htm
[3] https://www.cdc.gov/flu/season/faq-flu-season-2020-2021.htm
