Mary Madison, RN, RAC-CT, CDP
Clinical Consultant – Briggs Healthcare
I blogged early this week COVID-19 emergency declaration waivers. CMS revised and updated this information via MLN Matters Number: SE20011 on March 18, 2020.
This MLN Matters is a definite must-read. You’ll find updated information on Telehealth – look for the red ink on pages 4 and 5.
Telehealth Medicare can pay for office, hospital, and other visits furnished via telehealth across the country and including in patient’s places of residence starting March 6, 2020. A range of providers, such as doctors, nurse practitioners, clinical psychologists, and licensed clinical social workers, will be able to offer telehealth to their patients. Additionally, the HHS Office of Inspector General (OIG) is providing flexibility for healthcare providers to reduce or waive cost-sharing for telehealth visits paid by federal healthcare programs. Prior to this waiver Medicare could only pay for telehealth on a limited basis: when the person receiving the service is in a designated rural area and when they leave their home and go to a clinic, hospital, or certain other types of medical facilities for the service.
There are three main types of virtual services physicians and other professionals can provide to Medicare beneficiaries:
• Medicare telehealth visits • Virtual check-ins • e-visits
Plus:
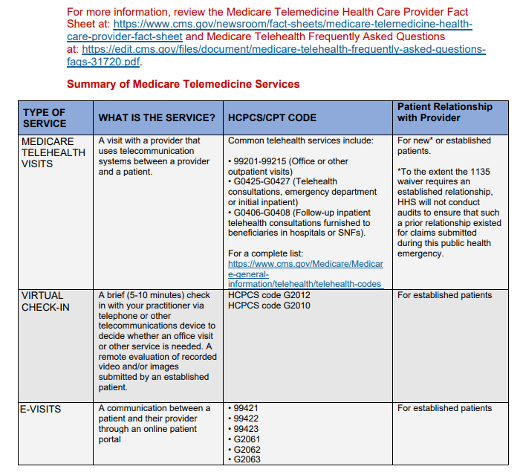
Access the MLN Matters SE20011 to see full screen information.
